Check out the full multimedia project here.
Young people are more stressed than ever, coming of age in a world that’s rapidly changing and drastically different than the one their parents grew up in.
That stress won’t disappear completely, but it isn’t all bad stress and there are healthy ways of coping.
UNDER PRESSURE
For Lexi Vincent, it’s cold sores. “Every midterm, every final,” the chiropractic student says, “I always get cold sores. Only then.”
Since he began medical school, Kushal Patel has lost more than 20 pounds. He’s a second-year student at Upstate Medical University in Syracuse, New York, a program he likens to “drinking from a firehose.”
And a few weeks ago, Alex Wysota, a Culver City visual effects editor, was diagnosed with a cyst on her thyroid. Like the mononucleosis that occasionally flares up, it came from work stress, she says.
Either doctor-confirmed or -speculated, all three believe their symptoms can be traced back to the extreme stress they’re under. And it’s very likely they’re right.
The body seeks to be in a state of constant homeostasis, carefully managed and adjusted. An article published in The Journal of the American Medical Association (JAMA) defined stress as “a state of disharmony, or threatened homeostasis.”
Stress arises from the gap between demand and capacity, according to Heidi Hanna, the executive director of The American Institute of Stress. Patel, Wysota and Vincent, with their demanding schedules balancing work, social lives and schooling, are exceeding their bodies’ natural capacity, i.e. putting them into stress.
A 2005 study, published in the Annual Review of Clinical Psychology, found that higher rates of stress linked to increases in smoking, substance use, accidents, sleep problems and eating disorders. Consistently high blood pressure damages arteries and increases plaque formation, which can lead to heart attacks or strokes.
A 2009 study out of Brazil published in the Clinics journal couldn’t find a direct link between ulcer diseases and stress, but did say that it was highly likely stress served as a trigger and modifying factor.
Patel, Wysota and Vincent are also all between 18 and 26, the ages associated with the developing theory of “emerging adulthood,” the period between adolescence and young adulthood.
First coined by Jeffrey Arnett in the American Psychologist journal in 2000, emerging adulthood is characterized as a period of identity explorations, instability, self-focus and possibilities.
The theory focuses on a transition between the relatively sheltered and cared-for adolescence and the stability of early adulthood. But when many of the tenets of young adulthood are foisted upon emerging adults, tension emerges.
And even beyond that, today’s young people are more stressed than ever, coming of age in a world that is rapidly changing and drastically different than the one their parents grew up in. The World Economic Forum wrote that the most in-demand occupations and specialties “did not exist 10 or even 5 years ago.” They estimated that 65 percent of children entering primary school today will end up working in jobs that don’t even exist yet.
A 2015 study published in the Social Science and Medicine journal noted that the cost of higher education has increased in the United States more than 250 percent over the past three decades against declining or stagnating wages; in 2012, student loans amounted to $1 trillion, second only to home mortgages.
WEAR AND TEAR
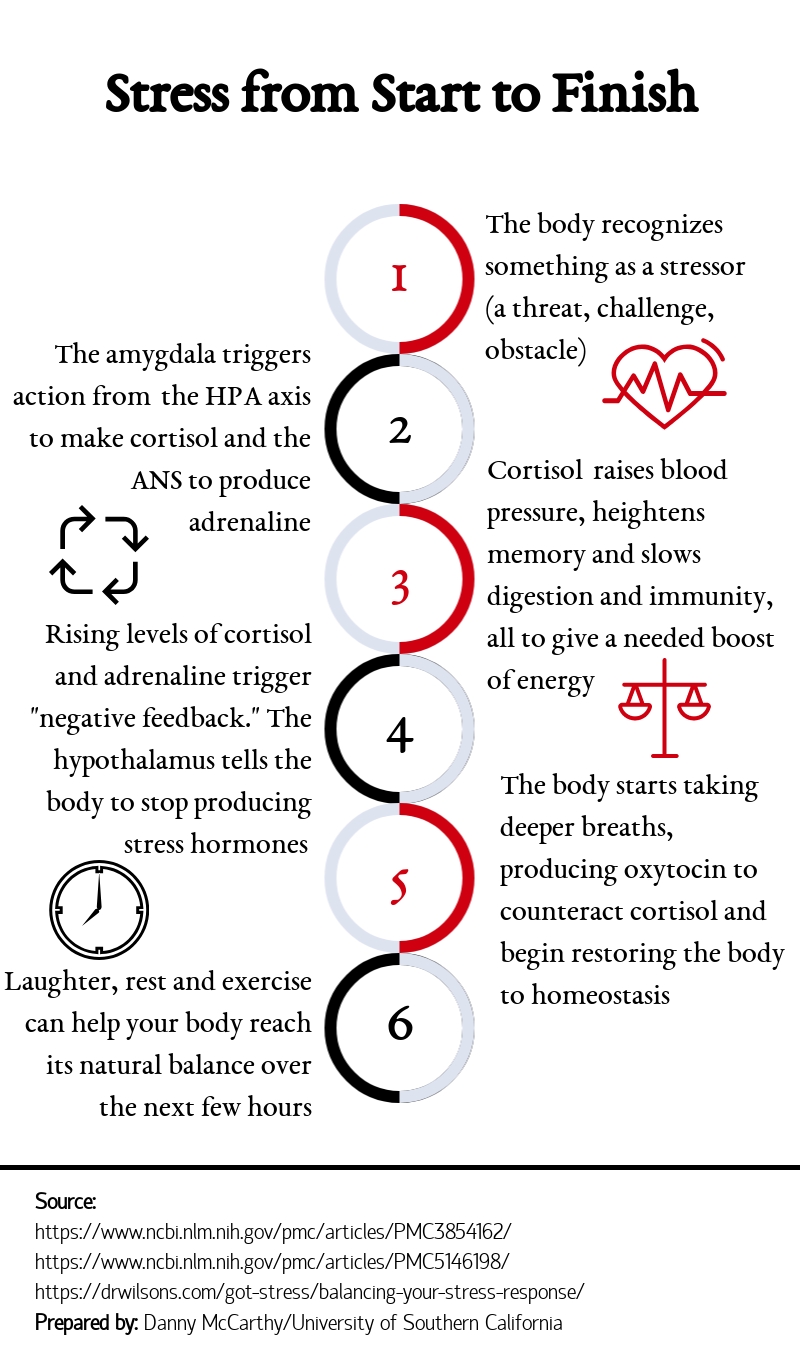
Stress falls into two categories: chronic or acute. Chronic stress affects the body much differently than acute and often has no finite end: financial difficulties or a prolonged terminal illness. Most of the stress that people face is acute, because it has, ostensibly, an ending eventually. For our ancient ancestors, acute stress might be a bear attack; in the modern age, it might be a challenging project at work.
Acute stress triggers sympathetic and parasympathetic responses from the system: the clinical terms for the “fight-or-flight” and “rest-and-digest” responses, respectively.
James Hébert, the director of the Cancer Prevention and Control Program out of the University of South Carolina, who has conducted research into how stress in minorities relates to cancer, has a simple, but effective, analogy.
“You’re making hot salsa, and you happen to cut yourself and the hot pepper juice gets into the cut,” he says. “The tissue gets bigger; it reddens, and what happens there is all of these different cells are being recruited to the site of the injury to repair the problem.”
The body’s reaction to acute stress is an inflammatory response that work in a similar way: it overrides the body’s other systems and puts all of its energy into confronting the threat, as reported in the 2005 Clinical Psychology study.
First, the amygdala recognizes a challenge and triggers a stress response from the hypothalamus. Through a cascading chain of commands and hormone signals, the hypothalamus activates the sympathetic response. Adrenaline, from the adrenal gland in the autonomic nervous system, is released, which is responsible for short spikes of energy. If the danger persists, cortisol is released from the hypothalamic pituitary adrenal (HPA) axis. Cortisol is slower to build, but it provides a longer stress response. Both work to increase blood sugar and break down fats for the promotion of energy.
Typically, within a few hours or days, the threat subsides. The problem comes from a rapid or continued series of acute stressors. The study found that “the acute stress response can become maladaptive if it is repeatedly or continuously activated.” Dr. Hébert confirmed as much.
“The literature on this is not as clear, but it seems to me that successive acute episodes can accumulate into a form of chronic stress,” he says. “So there isn’t a clean separation. It keeps happening over and over and over again.”
The Clinical Psychology study found that elevated levels of stress hormones associated with chronic stress also suppress immunity by directly affecting cytokine profiles. Cytokines are intercellular messenger molecules that signal activity to the immune system. Diminished cytokine activity means a diminished immune system, which is why you get sick more often while stressed.
As a chiropractic student at the Southern California University of Health Sciences, Lexi Vincent is pretty knowledgable about the science behind stress. “Stress is basically an excess of the hormone cortisol,” she says.
“In normal amounts, cortisol is good,” says Vincent. Spikes of cortisol are what get you out of bed in the morning, keeping you aware and aroused. However, high levels of cortisol can create an allostatic load, the continual “wear and tear” the body goes through under prolonged stress.
The combination of school and working full-time causes Vincent’s stress-induced cold sores. The small red blisters only last for a few days, but the resulting lesions can linger for as long as several weeks. Vincent has been getting these cold sores since high school, and has been on Acyclovir, a medication that’s used to prevent herpes sores and blisters, since she was 12.
Vincent touched upon some of the milestones of young adulthood as points of stress. “There’s more pressure for us to have all these things going on and have everything figured out,” she says, “job, life, what you’re doing and what you want to be.”
Despite the cold sores and stress, Vincent doesn’t see herself slowing down. “I always have my plate full,” she says. “When I’m not busy, I feel like I’m wasting time.”
LOVE AND FEAR
Stress itself isn’t a good thing or a bad thing, says George Elias, a psychiatrist in the University of Southern California’s Keck School of Medicine. “Stress is the unknown,” he says. “Without it, we’re not progressing.” He likens it to weight-lifting: stress builds (metaphorical) muscle.
A study out of the University of California, Berkeley found that short-term acute stress in rats actually improved the activity of the hippocampus, important for memory and emotion regulation, and increased “neurogenesis,” the formation of new neurons in the brain. The study also found that the improved memory they recorded in the rats could be attributed to that “stress-induced increase in neurogenesis.”
One of Vincent’s former professors, Laura Schmalzl, says the body is more than capable of dealing with stress. A stressor arises, the body reacts, the stressor goes away, and the body slowly returns back to normal.
Ideally, after the threat is dealt with, the body begins parasympathetic negative feedback to counteract the stress response. The “rest-or-digest” response slows the production of cortisol and increases the production of hormones such as vasopressin and oxytocin, to lower blood pressure and restore oxygen to the body’s systems.
Oxytocin and vasopressin, called the “peptides of love and fear” in the journal Psychiatria polska, can often counteract cortisol. Oxytocin, the same hormone released by positive physical contact, relaxes the body; vasopressin, a diuretic hormone, controls water conservation, as well as blood vessel constriction and expansion.
The problem is when the body is constantly triggered into sympathetic responses, and the counterbalance is never achieved.
“Most people these days are pretty much in sympathetic overdrive,” Schmalzl, a neuroscientist and yoga therapist, says. “If these things just happen momentarily in response to an outside stimulus, that’s okay. If that goes on over a prolonged period of time, your system is stressed all the time.”
Kushal Patel is well-versed in being stressed all the time, but found it came from an unexpected source.
Before he started medical school, Patel anticipated that the academics would be the most difficult part of the program. “There’s the slow, creeping up stress of ‘What if I don’t do well on this quiz?'” he says.
However, he quickly discovered that the social stress of medical school far outweighed the academic. With 170 people in his class, Patel described weird “high school” dynamics and antagonistic relationships. And even with his friends, there’s stress. “You want to do better [on quizzes] but you also want your friends to do well.”
The summer between his first and second years, Patel experienced his first panic attack. While that hasn’t happened since, Patel continues to face stress and a general lack of sleep, which is common among medical students.
A global study in the Journal of Clinical Sleep Medicine found that, compared to students in similarly rigorous programs such as law or economics, medical students had the highest instances of stress-disturbed sleep, insomnia and daytime sleepiness. In the United States specifically, medical students’ sleep was “significantly worse” than a healthy adult sample.
Patel didn’t compartmentalize his studies in his first year and didn’t take as much of an active role in his mental health. He says that he’s changed that now, and that when he and his friends go out, they’ve made a pact not to discuss school.
WHAT DOESN’T KILL YOU
Alex Wysota, who works as a special effects project manager in Culver City, called the past few months, “the most stressful months of my life.” She deflects from her stress almost on instinct. “I’m not saving lives,” she says, “I’m just pushing pixels around.”
However, while she doesn’t find the job particularly stressful, Wysota takes night classes in advanced Adobe Photoshop twice a week and constantly works long hours under various deadlines.
When mapping out how many hours she worked recently, she breaks out into raucous laughter. She had worked 95 hours in the last two weeks; her typical workweek averaged from 50 to 80 hours.
The stress was getting to her. Beyond the occasional mononucleosis flare-up, which made her sleepy all the time, Wysota recalls moodiness, nights spent crying, and a recently diagnosed cyst on her thyroid.
Wysota recognized that continuing on as she had been was not only unrealistic but also dangerous for her health. Her physical trainer recommended yoga, a suggestion Wysota took to skeptically. Until it worked.
She loves the physical activity as a method for alleviating her stress. “I would’ve packed up and gone home back to New York if I hadn’t started yoga,” she says. “It’s helped tremendously.”
Patel, Vincent, Hébert and Schmalzl also spoke highly of yoga as a way of increasing resilience to and coping with stress. Schmalzl, a trained yoga therapist, has even made it a point of research.
In an article published in the journal Frontiers in Human Neuroscience, Schmalzl found that two processes present in yoga therapy reduced psychological stress, inflammation and activity in both the HPA axis and sympathetic nervous system. She categorized them as “top-down,” setting intention and regulating attention, and “bottom-up,” modulating breathing and physical movement.
In conjunction, the two systems worked to increase self-regulation, “a conscious ability to maintain stability of the system by managing or altering responses to threat or adversity,” and increase one’s awareness of what’s going on inside the body.
The terms sound highfalutin but the reality is there. “Usually people only get aware that they’re stressed once their back gives out or they develop an actual psychosomatic problem,” she says. “We’re not aware because we’re constantly bombarded with external stimuli.”
Yoga practice, or more specifically the emphasis on self-regulation, trains the body to forget those external stimuli for a moment. “It allows your brain to process what’s happening in your system,” Schmalzl says. “If you don’t have very specific, self-regulatory tools…no wonder you’re stressed out.”
The Annual Review of Clinical Psychology study found that chronic stress stimulation led to sustained increases in blood pressure, and caused a tendency of confronting “to all types of stressors with a vascular response.” Schmalzl says that even a few minutes per day of quiet breathing, away from your cell phone, could drastically reduce your stress levels and drop your blood pressure.
Yoga isn’t the only way to reduce your stress. A study from the European Journal of Psychtraumatology found that Tetris helped people deal with post-traumatic stress disorder. And taking a few deep breaths could trigger activity from the parasympathetic nervous system, the “rest-and-digest” counterpart to “fight-or-flight,” and combat incoming stress.
It could also be as simple as a matter of curiosity, according to Heidi Hanna. She’s been researching how actively thinking of stress as curiosity can change the way your brain functions. “Essentially the neurons are switching to an “approach” mode as opposed to an “avoid” mode,” she says.
Hanna advocates for developing curiosity, and even creativity and humor, towards the things that normally would stress us out.
She has a point. Stress makes your body more reactive. As you get more stressed, your body is less equipped to handle it and flares up at the slightest obstacle. By swapping to curiosity, “the brain starts to notice things in a different way, in a different lens, and that can decrease the reactivity to the stress of our life,” she says. “We can adapt and cope effectively. We actually grow stronger as a result.”
Elias makes a similar argument, that short-term stress is actually positive.
“When astronauts are in zero-g, there’s no stress on their bodies. So when they come back to Earth, they actually come back weaker,” he says.
“The brain is the same way.”